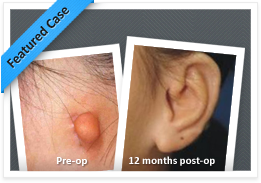
PATIENT RESULTS
FAQ’s
What is microtia?
Microtia is a birth deformity of the ear that occurs about one in 5,000-7,000 births, depending on varying statistics in different countries and in different ethnic races. When broken down in Latin, the term “microtia” is easy to understand. Micro=small; Otia=ear.
What is Atresia?
Atresia is absence or underdevelopment of the ear canal and middle ear structures. Microtia is almost always accompanied by atresia because the outer ear and the middle ear develop from one common block of tissue at the same time of development in the womb. Some microtia patients have what appears at first look to be a normal canal, but many of them are a “blind alley.”See handout on aural atresia for more info.
At what age should a hearing test be done ?
Hearing testing should be done soon after birth and every 12 to 18 months thereafter. This is most important in unilateral microtia/atresia to make sure the normal/unaffected ear is hearing well. It is vital to keep the unaffected ear healthy by treating any ear infections early.
What causes microtia ?
The exact cause (etiology) of microtia is unknown. It may be due to a problem with a blood vessel blockage early in development of the child before birth and is not thought to be due to anything the mother has done or taken in pregnancy.
What is the risk of recurrence of microtia within the family and what are the chances that a microtia patient could also have children with microtia?
The incidence of microtia is one in 5-7,000. Parents who have a child with microtia then have an increased risk of 1 in 20 for subsequent children. The risk of a child with microtia eventually having a child of his/her own with microtia is also one in twenty.
What other medical problems are associated with microtia?
The majority of patients with microtia have no other problems aside from the ear. Approximately 50% have underdeveloped bony and soft tissues on the involved side of the face (hemifacial microsomia) and 15 percent have facial nerve weakness. Other general abnormalities such as cleft lip, cardiac, or urological problems are encountered much less frequently.
When does a child with microtia become aware of it?
Children with microtia become aware of their differences at about 3-4 years of age. Typically, they start comparing sides in a mirror and begin referring to their microtia as their “little ear “ but remain unconcerned by this difference. Awareness of facial difference between children starts around 5 years of age and an ear deformity may attract innocent curiosity at this age from peers. Teasing is almost unheard of in our experience with microtia but if it occurs it is not until 8-12 years of age. More commonly it is a desire to fit in that manifests around 10-12 years of age in most children with microtia and leads to a request for reconstruction. However close to 25% of patients live normal lives with their microtia/atresia and never request surgery.
What should the parents tell their child with microtia when they discover that they are “different”?
When the child discovers that he/she has a small ear, parents should tell the child that he/she was born with a small ear, and that the doctor is going to make it larger when the child is older. From then on we recommend that parents then treat the child as absolutely normal and not make a “big deal” about it. The only children we have ever seen bothered about their microtia before the age of 7 or 8 are those whose parents are not coping well with the problem or accepting of it. Children with microtia rarely will need a psychologist but in general parents are the best psychologists for their children. Providing your child with a few key explanations for their ear shape difference will stop simple curiosity from other children proceeding to teasing in most cases. Interestingly and in contrast to microtia we see frequent episodes of teasing from the age 7-8 in children with two normal ears that stick out (“bat ears”) .
At what age can microtia be repaired?
We generally do not operate on children with microtia before the age of six for two reasons: for rib graft reconstruction the technical reason is to allow the rib cartilage to grow large enough for carving an ear to match the opposite side and to avoid causing a deformity of the chest wall ; more importantly the psychological reason for waiting is that a child with microtia is neither concerned about the problem nor very cooperative before then. This makes post-operative care very difficult on the child and all those involved in their care (parents, doctors, nurses). We feel it is important for the child to be old enough to understand and personally “consent” to having the surgery. What if the surgery goes badly or the outcome is poor ?The child has to live for the rest of their life with a problem from an operation that they did not ever consent to .
Even though surgery can be started as early as 4-5 years with Medpor and 7-9 years with rib we rarely encounter patients requesting surgery at these ages but we frequently encounter parents requesting surgery on their children well before this !
What are the current methods being used to correct microtia?
The two main methods for repairing microtia rely on different sources for the ear framework. One method uses a living sculpture from the patient’s own tissues (rib cartilage) and the other uses a framework of firm artificial plastic covered in a “living membrane” plus skin grafts (Medpor). This spells out the main difference between the two techniques: one type of ear is created from your own bodily tissues whereas the other is an ear of a combination of foreign material and the patient’s own tissues.
Does a surgically constructed ear grow?
Ears created from the person’s own rib cartilage are alive but there is no evidence they grow.Ear frameworks made from plastic /Medpor obviously can’t grow because they are not alive. Growth of a reconstructed ear is not important since generally by 5-6 years of age the normal unaffected ear is close to its final adult size so an adult size ear can be made without concern for future growth.
What are the advantages of correcting microtia with living tissue?
The advantage of correcting microtia with one’s own tissue is obvious. The new ear is sculpted from the patient’s own cartilage and skin and therefore is alive, grows with a child, and heals without problems. This allows a person to resume normal sports, swimming, and PE activities 4-6 weeks after surgery with no particular concerns. The pioneer Burt Brent has reconstructed ears for more than 1,500 patients with microtia and has followed a number of them for more than 30 years. Ears constructed by this method retain their form and have withstood the test of time—they should last a lifetime.
Are there limitations of sports activities that patients can perform after microtia repair?
Irrespective of whether Rib or Medpor is used we do not impose limitations on activities after an ear reconstruction has healed. Australian children are particularly active in sports and often contact sports and any reconstruction needs to be able to withstand these activities. Rib cartilage is proven to resist every imaginable trauma and contact sports are permitted without extra protection or restriction. At this stage there is less than 20 years long term follow-up with Medpor ears internationally and it is not known exactly how they will withstand trauma or whether a Medpor ear will be forever. Early results are encouraging but even 20 years is not long considering we are operating on young children with their whole lives ahead of them.
How much discomfort is there when using rib cartilage to reconstruct ears in children?How does this compare to Medpor ?
The ear itself is hardly painful at all and the rib donor site is the main source of pain. However in the last five years avaiiability of new technology in the form of Pain Buster pumps has dramatically reduced or eliminated this issue and we routinely use these for the first 24-48 hours after surgery. A Medpor procedure also involves some discomfort but mostly from the extensive raw area of scalp where the large skin graft is taken from. Simply pain medications will control this well but there is some discomfort still. With both options there is some minimal discomfort involved in removing the bandages /dressings 4-7 days later and this requires a fully cooperative child to tolerate this .
Can one use a parent’s rib cartilage or tissue from another person or animal just like with other organ transplants ?
Attempts at using cartilage donated by mothers to their children were made in the 1930s but all resulted in poor results due to rejection.
Because tissue other than your own is a “foreign material,” to ensure success of organ transplants, a patient is required to take special drugs for the rest of his/her life to prevent rejection of those organs. The dangerous side effects of these drugs are worthwhile risking for a life saving procedure such as a heart or kidney transplant but not for a non life-threatening condition such as microtia.
How durable are reconstructed ears ?
Rib cartilage reconstructions have now long been proven as durable over more than 50 years of follow up and as such remain the gold standard in Europe, the USA, and Australasia. They can withstand most sorts of trauma and there are no restrictions on patient activities or requirements for extra protection in contact sports. The durability of Medpor is likely to be very good also but it is as yet less proven in this respect simply because there is not long term follow up beyond 20 years . Patients undertaking Medpor reconstructions simply need to be aware that we cannot guarantee it will be an “ear for life”. In addition being a foreign body it may always have a slight risk of becoming infected and needing to be removed at anytime in the future. Major septic bacterial illnesses or wounds /insect bites over the implant or ner it are an ever present risk although the real risk is probably very low.
Tissue engineering of ears: Is this the future?
For many years there has been considerable interest in creating a “pre-fabricated” framework from autogenous cartilage in order to circumvent the necessity to fabricate an ear framework with complex reconstructive surgery. Recently, interest in this “pre-fabrication” concept has been rekindled via modern “tissue engineering” techniques in which cartilage cells are grown in the laboratory and seeded upon a synthetic ear form which is then implanted beneath the skin of a mouse.The early results are interesting but the work is not being carried out under the same conditions as in a human ear reconstruction; the researchers’ frameworks are being placed under the very loose skin of a mouse’s back, whereas in human ear repair, the new framework must be placed underneath snug skin just in front of the hairline in the ear region. Unlike the loose skin of an animal’s back, that skin is very tight and will flatten out any framework that consists of flimsy material. Currently it seems likely that this sort of option is many decades away from being a reality.
OUR LOCATION
REQUEST AN APPOINTEMENT
After submitting the form above, you will be contacted by our staff to answer any questions and discuss scheduling an appointment. You can also call us directly at +61 3 9508 9508 or Lee Dowling PA to Dr Greensmith on leed@melbplastsurg.com.